How to Submit a Claim on StoriiCare
This article walks you through selecting invoices, submitting them as claims for reimbursement, and tracking their status from the Claims tab.
1. Filter and Select Invoices
Open the Billing feature.
Select the Invoices tab.
Use the available filters to narrow down the invoices you want to include (filter by payor, participant, or date range).
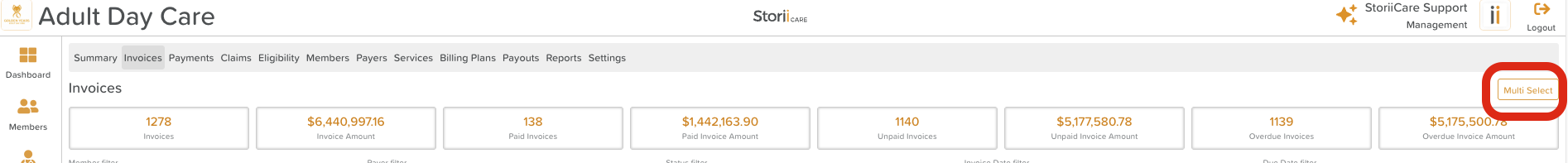
Once filtered, click Multi Select in the top right-hand corner
Check the box next to each invoice you want to include in your submission.
2. Submit the Claim(s)
With your invoices selected, click Bulk Actions in the top right-hand corner
From the dropdown menu that appears, select either Submit 837P or Submit 837I, depending on your organization's setup. If you're unsure which applies to your organization, check with your billing administrator or review this article.
Once processed, the submitted invoices will be accessible from the Claims tab.
3. Track and Manage Claims
Navigate to the Claims tab within the Billing section to monitor your submissions. From here, you can:
Track the status of each submitted claim
See which invoices are attached to a claim
View denial details for any claims that were not accepted, prior to resubmitting
Claim Status Overview
Here is a key explaining what each claim status means:
Paid — The claim has been processed, and payment has been issued by the payer.
Denied — The claim was processed but rejected by the payer. The client should review the denial reason and resubmit or appeal.
Accepted — The claim passed initial validation and is in the payer's queue, but not yet fully processed.
Acknowledged — The claim was received and acknowledged by the payer/clearinghouse. This is an early-stage confirmation before full processing begins.
Processing — The claim is actively being reviewed by the payer. No action needed yet.
Not Found — The payer has no record of the claim. There could be a submission error or timing issue. It is worth investigating and potentially resubmitting. Reach out to StoriiCare or Stedi for support, if needed.
Search Failed — The system couldn't retrieve a status. Likely a technical/connectivity issue rather than a payer decision — Stedi or StoriiCare may need to be looped in.
Error — Something went wrong during submission or processing. This could indicate a data or formatting issue. This typically requires StoriiCare or Stedi to investigate.
Need More Help?
If you need further assistance, you can reach out to our support team by emailing support@storii.com. Our support team is ready to help you with any questions or issues you may have.